Finnish doctors are taking creative, patient-oriented approaches to defeating a growing public health problem.
“I sometimes say that I’m the most indebted doctor in Finland,” says Timo Joensuu, sitting in the conference room of the two-year-old Docrates cancer hospital in Helsinki. Built on a seaside property with help from corporate investors, contributions from friends and loans taken out by Joensuu himself, the hospital has established itself as a model for patient-oriented cancer treatment.
The concept for Docrates, whose name is a hybrid of the words “doctor” and “Socrates,” arose from Joensuu’s frustration with a patient care model in which doctors stay at an authoritative distance and patients often have to wait for weeks or months before beginning treatment. In diseases such as pancreatic cancer a two-month delay can be critical, and with slower-moving cancers waiting for weeks can result in added distress.
At Docrates, treatments often begin within 24 hours from diagnosis and doctors and nurses answer calls from patients around the clock. A built-in health centre offers services including exercise and nutrition programs, makeup coaching, massages and acupuncture. Hospital rooms look out over the ocean, and Docrates’s sunny lobby, void of the smell of disinfectants, is decorated with colourful designer chairs.

Docrates’s sunny lobby, void of the smell of disinfectants, is decorated with colourful designer chairs. Photo: Docrates
“Socrates believed that people could grasp the truth by thinking for themselves, and we practice the same way of thinking with our patients,” says Joensuu. “We offer personal support and make sure that they are informed. We can never fully predict which treatment is best for each patient, and a doctor-patient relationship is crucial in finding that out.”
About 24,000 people in Finland are diagnosed annually with cancer. As its prevalence continues to grow, its individualistic nature becomes all the more obvious; cancer appears in countless types and subcategories, each of which responds to a different cocktail of treatments and medications. Due to its inherent mysteries, cancer also leaves behind a trail of uncertainty in communities of patients and survivors. In recent years, forward-thinking Finnish institutions such as Docrates have begun to employ a personalised approach to both patient care and the development of new treatments. The emerging trend of personalised medicine can further brighten Finland’s position on the global scientific map.
A rich resource
One of Joensuu’s motivations for building a new hospital was his realisation that the public sector did not yet have enough resources to optimise cancer treatment for each individual patient. He collected his first million euros from independent investors, colleagues and friends, and the hospital’s construction was paid for by the life insurance division of Nordea Bank. Docrates is still entirely in Finnish ownership; its largest owner is Lääkärikeskus, a large chain of private medical centres in Finland.
“In building Docrates we’ve already proven that we can attract tens of millions of euros into cancer research and treatment. In short, we can provide a giant additional resource for this particular field of medicine,” Joensuu says. “Everyone is worried about where the resources for cancer treatment will come from, and a private hospital like this one is a huge opportunity.”

At Docrates in Helsinki, treatment is more personalised and patient-oriented than at many other cancer hospitals. Photo: Docrates
Joensuu currently works from about six in the morning to eight in the evening, and continues to answer patient calls around the clock. Six full-time doctors currently work at Docrates, which has so far treated patients from about 25 countries. The clinic has become known internationally by offering the latest treatment options and equipment in one facility. It has, for example, a cyclotron particle accelerator, a GMP laboratory for handling radioactive substances and state-of the art radiation and imaging equipment.
“We’re not missing anything, so we can optimise treatment in a way that takes into account all different scenarios on the patient’s part,” Joensuu says.
“Our doctors seem to come back from each conference with three or four new treatments,” says Docrates nurse Jenni Keinänen. “Although I can’t say that one should never give up hope, there is quite a bit of it; even if we aren’t able to cure the cancer, we can increase our patients’ quality of life.”
Decoding treatments
Beyond patient care, a different kind of effort to personalise the treatment of cancers is underway at the Institute for Molecular Medicine Finland (FIMM), run by the University of Helsinki. The institute has begun to make use of Finland’s strong track record in biobanking and genetics to develop ways to determine the best treatments for cancer, cardiovascular diseases and other illnesses.
Most recently, professor Olli Kallioniemi’s research group has begun to apply molecular-level information to the treatment of leukemia. These personalised treatment methods have already been employed in a handful of patients, and clinical trials on individualised leukemia care are expected to begin in 2012 in collaboration with hematologists at the Helsinki University Hospital.
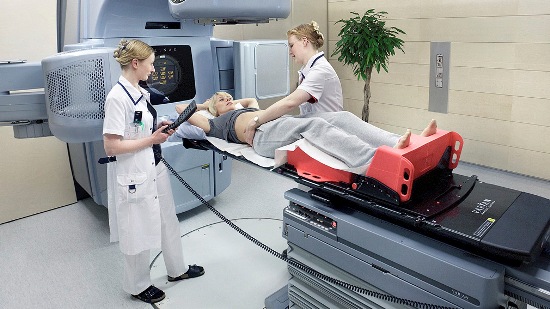
Nurses help prepare a patient for a form of radiation treatment. Photo: Docrates
“In the future, public health will make even greater use of genetics – if you have, say, a cardiovascular disease, your doctor would look at your genetic profile in addition to traditional risk factors. Cancer, though, is a completely different ballgame,” says Kallioniemi. “Cancers are very individual to begin with; they are entities with their own molecular profiles that mutate and evolve. However, we can look at genetic profiles to see how a patient will respond to a particular cancer treatment.”
One of the largest challenges in taking cancer treatments in a new direction is convincing decision-makers to veer from long-standing treatment regimens.
“Instituting a new treatment method requires a lot of work because existing strategies have such a long-standing foundation,” says Kallioniemi. His group began doing work with advanced leukemia patients because the field has already been employing immunology and genetic testing in diagnostics and treatment selection for years. The clinical trial will be conducted in patients with advanced, treatment-refractory cancers, as introducing alternative treatments as the first line of therapy can be risky. After personalised medicine has been shown to be effective, it can be introduced to patients suffering from less advanced cancers.
“Of course we have to move gradually, and as we gather more information on a molecular level, we learn to interpret it better and use it to select the best treatments for each individual patient,” Kallioniemi adds. “We don’t yet have a simple answer to how we can employ our approach to the population at large because our health care system it’s not yet ready for individualised medicine. But this is the direction in which cancer treatment is headed.”
By Laura Palotie, October 2011



